I wrote this article a few years ago.
It seems particularly relevant now.

Recent news has highlighted the restrictive financial environment that maternity units will be expected to operate in.
Yet, at the same time midwives are charged with the important task of improving the quality of care and services.
David Cameron has said, “The whole aim of these NHS reforms is to make sure we get the value for the money we put in.”[1]
In the same article, Stephen Dorrell, former Health Secretary commented that, “In real terms, the NHS budget was being broadly maintained, but we’re having to find ways of doing more with the same amount of money.”[2]
The only way of improving maternity services is by optimising facilities, saving money wherever practical and normalising childbirth to a far greater extent.

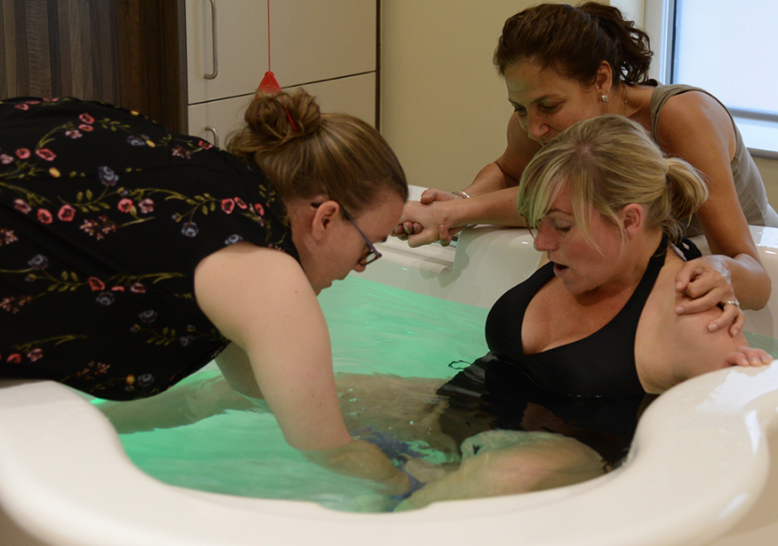
Studies have shown that women who are supported during labour need to have fewer painkillers, experience fewer interventions and give birth to stronger babies.
After their babies are born, supported women feel better about themselves, their labour and their babies.
A focus on normalising birth results in better quality, safer care for mothers and their babies with an improved experience.
Increasing normal births is associated with shorter (or no) hospital stays, fewer adverse incidents and admissions to neonatal units and better health outcomes for mothers.
It is also associated with higher rates of successful breastfeeding and a more positive birth experience.
These changes benefit not only women and their families but also maternity staff. Midwives are able to spend less time on non-clinical tasks and more on caring for women and their babies.
Psychologically speaking, and in particular for first time mothers, the less intervention and a more hands on approach with one-to-one support means that mothers will leave hospital feeling held and therefore far better prepared for motherhood.
This again has a domino effect, not just on the welfare of the infant, but also circumventing the need for costly government and LA interventionist approaches in particular for younger mothers post-partum.

What increases the likelihood of normal births?
It is also known that some factors help to facilitate straightforward birth without evidence of additional risks, including one-to-one support, immersion in water for low-risk women, planning for a home birth, care from known midwives, more extensive training of junior doctors, employment of consultant midwives focusing on normality, and support on the labour ward from consultant obstetricians[3].
How can midwives make a case for purchasing birth pools?
The need for more water birth facilities is evident. The problem is that financial controllers are under pressure to save money.
They will not be easily convinced of the necessity unless you clearly stress that purchasing pools should not be viewed as a cost but rather to make the case that they are a valuable investment and will enable your unit to optimise resources, improve the quality of care and yield a return of significant financial savings.
A birth pool is a simple, inexpensive piece of medical equipment that can have a major impact on the quality of care and cost of having a baby.
The bed is no longer the primary focus of the room: having birth pools in hospitals and delivery suites facilitates pain relief encourages relaxation and therefore confidence and promotes mobility along with soft furnishings such as beanbags.

Importantly, this results in significant financial savings!
Our cost study has revealed that savings of up to £700.00 per birth can be achieved.
For example, St Richards Hospital in Chichester has three of our birth pools as well as our soft furnishings.
They recently reported their first successful VBAC in the pool for a woman who had previously had twins by c-section.
Depending on complications, a c-section costs between £1,370 and £1,879 in contrast to a normal delivery that is usually between £735 and £1,097.[4]
The experience of hospitals that have birth pools demonstrates that the cost of installing a pool is soon recouped by the savings achieved through reduced use of medical methods of pain relief and shorter hospital stays.
Wherever possible, women should have the opportunity to labour in water, as this is often far more comfortable.
The NHS has advised hospitals to ensure facilities are in place for this: three pools for 1,000 births a year is seen as adequate provision[5].
[1] BBC: 19/01/11
[2] BBC 19/01/11 taken from BBC Radio 4 Today programme
[3] Hodnett ED, Gates S, Hofmeyr GJ, Sakala C. Continuous support for women during childbirth. Cochrane Database of Systematic Reviews 2007, Issue 3. Art. No.: CD003766. DOI: 10.1002/14651858.CD003766.pub2
[4] NHS Institute, 2009
[5] NHS Guidelines on Childbirth 26 September 2007









