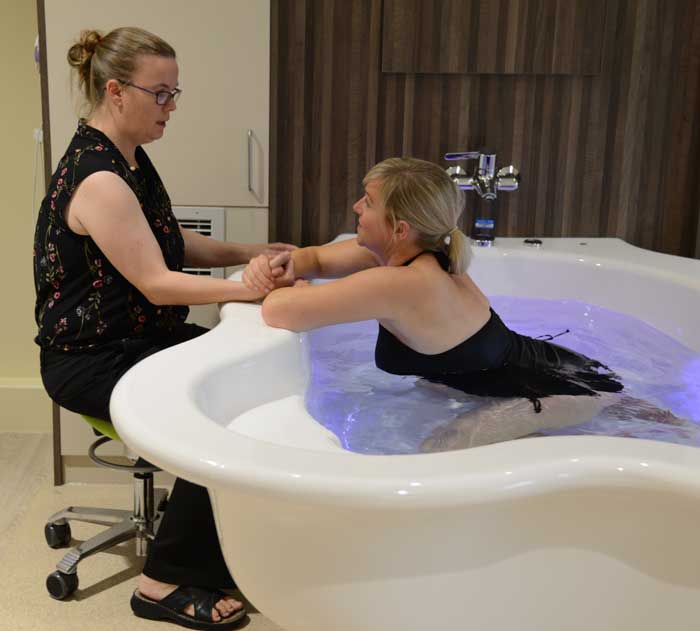
Water births provide “clear benefits” for healthy mothers and their newborns, with fewer interventions and complications during and after the birth than standard care, researchers believe.
Analysis of the available evidence also found that water births result in higher levels of satisfaction for mothers. A water birth involves using a birthing pool to achieve relaxation and pain relief, either exiting the pool for the birth, so the baby can emerge into air to breathe, or remaining in the birthing pool for the birth, bringing the baby to the surface to start breathing.
The Oxford Brookes University researchers compared the extent of healthcare interventions needed during and after labour between the two different types of water birth and to see if outcomes differed between a water birth and standard care – without the use of a birthing pool. They analysed 36 studies published between 2000 and 2021 involving 157,546 women.
The studies included a broad range of interventions and outcomes, including induced labour, artificial breaking of waters, stimulation of labour and epidural use among many others.
Data analysis of the study results showed that a water birth, regardless of whether women birth in or out of the pool, “has clear benefits to women” in obstetric units, where most births take place and where healthcare interventions and complications are more probable than in midwife-led units, note the researchers. A water birth was as safe as standard care for healthy mums and their newborns.
Compared with standard care, a water birth significantly reduced the use of epidurals, injected opioids, episiotomy, as well as pain and heavy bleeding after the birth. And it increased mothers’ satisfaction levels and the odds of an intact perineum. And there was no difference in the rate of C-sections, the Oxford Brookes University researchers found.
“Water immersion can significantly increase the likelihood of an intact perineum and reduce episiotomy, an intervention which offers no perineal or fetal benefit, can increase postnatal pain, anxiety, and impact negatively on a woman’s birth experience,” they concluded.
There were more instances of umbilical cord breakage among water births, but the rate was still low: 4.3/1000 births in water compared with 1.3/1000 births with standard care. This may be linked to pulling on the umbilical cord when the newborn is brought up out of the water, the researchers suggested.
They acknowledge that information on birth settings, care practices, interventions and outcomes varied considerably among the studies, and few were carried out in midwife-led units or in the mother’s home, which may have affected the findings of analysis.
But they conclude: “Water immersion provides benefits for the mother and newborn when used in the obstetric setting, making water immersion a low-tech intervention for improving quality and satisfaction with care.
“In addition, water immersion during labour and water birth alter clinical practice, resulting in less augmentation, episiotomy, and requirements for pharmacological analgesia. Water immersion is an effective method to reduce pain in labour, without increasing risk.”
The researchers, who publish their findings in the journal BMJ Open, called for future research to include factors that are known to influence interventions and outcomes during and after labour and birth. These include how many children a woman has already had, where she gives birth, who looks after her, and the care she receives, they said.